
 Lost Souls Lost Souls
|
 Peds Atlas Peds Atlas
|
 Volumes Volumes
|
 Aortic Diameter - Adult Aortic Diameter - Adult
|
 Kidney Size - Peds Kidney Size - Peds
|
 Spleen Size - Peds Spleen Size - Peds
|
 Testicular Volume Testicular Volume
|
 Lung Nodule 2017 Lung Nodule 2017
|
 Contact Contact
|
Depth Correction Calculator for Nuclear Medicine Split Renal Function
Enter Parameters Above and click Calculate to see the Results.
Need for Depth-Correction
- Even small asymmetric differences in the distances between the skin and the kidneys can have a substantial effect on 𝛾-photon absorption by the overlying soft tissues, and can adversely affect the accuracy of the measured split renal function. Such depth asymmetries are common. For example, a 2 cm difference in depth would cause a falsely asymmetric measurement of 57.2% - 42.8% due to photon absorption and scattering, even if the true function of both kidneys were exactly equal 50% - 50%.
Methods
- Depth-correction to the measured split renal percentages is calculated by dividing the measured scintigraphic counts by the fraction of photons that penetrate from the kidneys to the skin surface due to absorption effects, and expressing each kidney corrected counts as a percentage of the sum of bilateral renal corrected counts. Report text is generated.
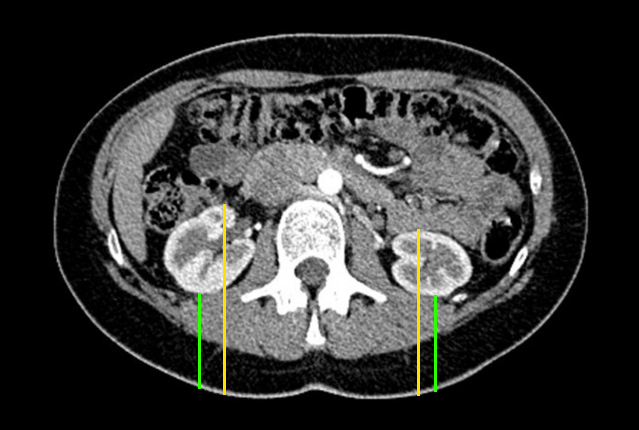
- To calculate the fraction of photons that are absorbed, each kidney is approximated as a 3D ellipsoid with major axes aligned orthogonally with the gamma camera, with size and depth specified by input parameters, which are typically measured on a prior CT or MRI. Thickness of the renal cortex can be specified, or a default value of 1 cm can be used, which this method treats as a thickness between concentric ellipsoids that are centered on the same point. Precise value of cortical thickness has negligible impact on depth-correction, but may be of significance if additional calculation of renal function per gram or per cm3 of renal tissue is desired.
- Radiotracer distribution during the initial phase that is used for split renal function calculation is approximated as homogenous throughout the volume of the cortex, or if cortical thickness is omitted, throughout the entire kidney.
- The concept of effective cortical thickness throughout which radiotracer is distributed assumes different meaning depending on the time since injection of tracer. Based on IV-contrast studies, typically angiographic or corticomedullary phase appears 25 - 80 seconds after injection during which the effective cortical thickness of radiotracer distribution is relatively thin. Nephrographic phase is present approximately 90 seconds after injection, during which the effective cortical thickess would approximate entirety of renal soft tissue thickness. Pyelographic or excretory phase occurs approximately 3 minutes after injection.
- Nuclear medicine split renal function measurements are typically obtained from images acquired during first 1-2 minutes after radiotracer injection.
- Each kidney ellipsoid is divided into numerous thin elliptical slices that are oriented in the coronal plane, parallel to the plane of the camera, with a central elliptical hole if the slice plane traverses central hilar elements that do not constitute cortex. 200 slices are used by default. The length and width of the kidney in the coronal plane have only a minimal effect, and are therefore not needed as input parameters, unless the additional calculations are desired that involve cortical thickness, or split renal function per cm3 of renal tissue.
- A fraction of photons that originate within each of these slices will penetrate through both the overlying portion of the kidney and tissues posterior to the kidney, and will be detected by the gamma camera. This fraction is calculated using appropriate linear attenuation coefficients for 140keV photons that are produced by Tc-99m based tracers, and optionally using densities of the overlying tissues. Photon loss due to camera inefficiencies is assumed to be symmetric, and therefore does not affect split renal function percentages.
- Adipose Tissue: density 0.9 g/cm3, Linear Attenuation Coefficient at 140 keV (μ/ρ) 0.15376
- Muscle Tissue: density 1.0597 g/cm3, Linear Attenuation Coefficient at 140 keV (μ/ρ) 0.15322
- Kidney Tissue: density 1.0597 g/cm3, Linear Attenuation Coefficient at 140 keV (μ/ρ) 0.15322
- The overall fraction of photons that arise from each kidney and penetrate through the tissues is calculated as a sum (integral) of each coronal slice volume and resulting absorption by overlying tissues.
- This method assumes that absorption is the dominant effect, and that spatial effects are minimal in the presence of collimator and large detector size.
- Decrease in the detected photons with distance is generally due to a combination of two effects: interaction of photons with soft tissues and spatial effects. Interaction with tissues is considered the dominant effect in this setting and in this calculator.
- Photons can be absorbed according to Beer-Lambert Law, and scattered into lower energies that are not detected by the camera.
- In other geometries, purely spatial effect arising from a fraction of randomly-oriented photon trajectories intersecting the area of the detector typically results in decrease of the number of detected photons with distance. Calculation of photon flux decrease due to increasing distance is non-trivial. Inverse-R2 effects of distance on photon flux apply only to geometries that approximate a point-source and point-detector separated by a large distance in relation to their sizes. The geometry of the gamma camera is substantially different, as the detector size is large in relation to the distance to each kidney and large in relation to any asymmetries in kidney depths. The typical size of a kidney is also significant in relation to its distance to the detector. In air or empty space and at small distances, this large detector size would more closely approximate the geometry of a point source emitting photons that impact an infinitely large plane detector. An extremely large or infinite planar detector would be distance-invariant in empty space, as 50% of emitted photons would strike the detector regardless of distance from the source. Parallel-hole collimators approximately preserve this distance-invariant effect to some extent, though with small fluctuations as a function of distance very near the collimator surface; point sources that are farther away have additional straight paths to detector surface through more neighboring collimator holes, therefore resulting in effectively increased surface area of the detector as distance increases; For typical distances of multiple centimeters, the ratio of this exposed detector surface area to the surface area of a sphere centered at the point source and its radius reaching the detector is approximately constant regardless of distance, therefore capturing a constant fraction of emitted photons. For point sources located within soft tissues, photon absorbtion on trajectories that are at an oblique angle to the detector would be higher as these traverse more tissue, and therefore photon flux would indeed decrease with distance. However, typical collimators nearly completely reject photons that deviate more than about 7 degrees from perpendicular, and expose a diminishing area of the detector surface at the bottom of the collimator hole as the angle of incoming photons is increased from the perpendicular. The difference in path lengths through tissues is negligible between photons that impact the detector at 90-degrees or 97-degrees, with the 97 degree photons traversing only 0.75% longer path.